5 Capnography Use Cases That Standardize Your Clinical Practice
1. Confirmation of Proper Endotracheal Intubation
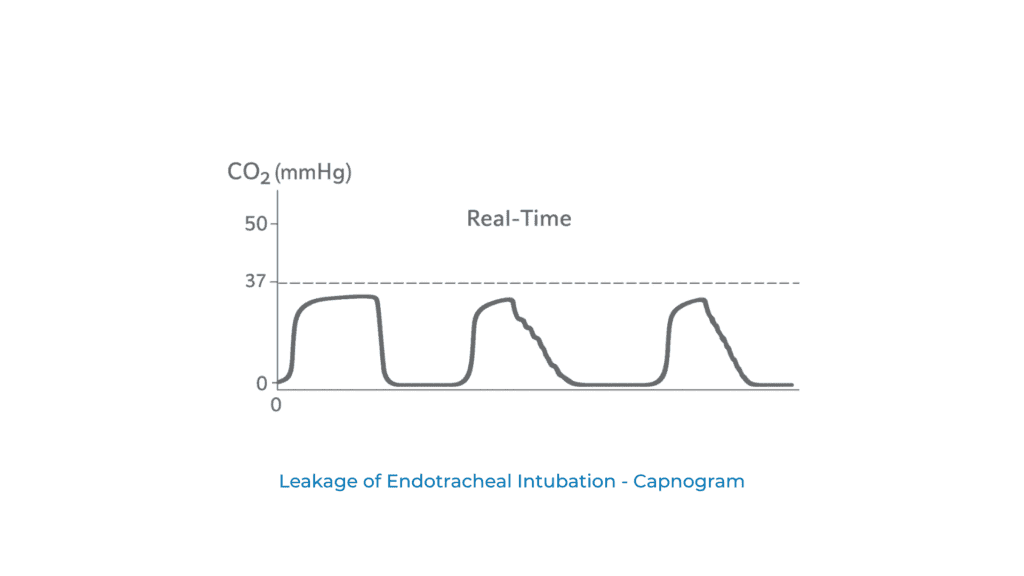
Intubating a patient is an everyday task for anaesthesiologists and critical care specialists. It is often challenging.
Clinical signs alone may be unreliable, particularly in difficult airway situations.
Continuous waveform capnography provides immediate confirmation of tracheal intubation by detecting exhaled CO₂.
Leakage around the endotracheal tube may produce a waveform pattern as shown.
It is considered a standard method according to the AIDAA 2016 Guidelines.
2. Anaesthesia Monitoring and Ventilation Assessment

Capnography waveforms provide valuable insight into patient-ventilator interaction.
The shape of the capnogram helps clinicians recognize patterns such as curare cleft, hypoventilation, hyperventilation and bronchospasm.
It provides more than numerical monitoring. It enables early adjustment of ventilator settings, prevention of respiratory complications, and optimization of anesthetic depth.
The attached graphs will help you to interpret ventilation quality;
3. Detection of CO2 Retention During Laparoscopic Surgeries
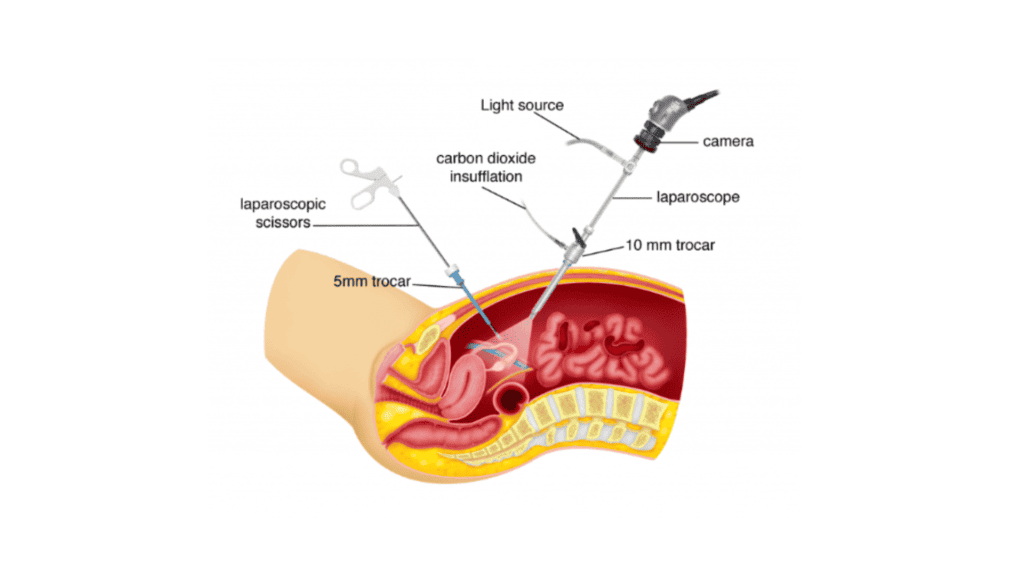
During laparoscopic procedures, insufflated CO₂ may be absorbed int systemic circulation, increasing arterial CO₂ levels.
Capnography enables continuous monitoring of these changes and guides ventilation adjustments accordingly.
Clinical Benefits:
- Early recognition of hypercapnia
- Timely ventilatory correction
- Prevention of respiratory acidosis
- Improved intraoperative stability
Real-time ETCO₂ trends assist anaesthesiologists in maintaining appropriate ventilation throughout prolonged procedures.
4. Early Apnea Detection

Apnea may occur during sedation, recovery, or critical care management and can precede oxygen desaturation.
Unlike pulse oximetry, which reflects oxygenation delays, capnography detects cessation of ventilation immediately.
Clinical Benefits:
- Rapid identification of respiratory arrest
- Faster intervention
- Reduced risk of hypoxic injury
- Enhanced monitoring during procedural sedation
Early detection allows clinicians to intervene before significant physiological deterioration occurs.
5. Assessment of Spontaneous Breathing After Extubation
Following extubation, careful monitoring is required to ensure adequate return of spontaneous respiration.
It provides continuous confirmation of respiratory effort and ventilation adequacy.
Clinical Benefits:
- Detection of hypoventilation
- Monitoring respiratory recovery
- Support for safe postoperative care
- Increased confidence during recovery monitoring
Continuous CO₂ monitoring helps ensure smoother and safer transition from mechanical ventilation to spontaneous breathing.
Conclusion
Capnography extends monitoring beyond traditional vital signs by providing continuous, real-time insight into ventilation and respiratory physiology. Its ability to detect respiratory compromise early supports faster clinical decisions and improves patient safety across perioperative and critical care settings.
As capnography becomes increasingly integrated into routine clinical practice, it plays a vital role in enhancing respiratory monitoring and improving patient outcomes.









